Prevent Infection, Overdose, and Death
Harm reduction includes principles, policies, and practices that aim to reduce the harms associated with certain risky behaviors. Using harm-reduction strategies keeps us safe. For example, driving a car or riding a bike can be risky. However, if we wear our seat belt or helmet (two harm-reduction strategies), we are less likely to sustain severe injuries if we get in an accident.
Harm reduction strategies are also applicable to substance use and related social conditions. Grounded in public health, social justice and human rights, harm reduction strategies aim to promote positive behavior change by meeting people where they are at—without judgement, coercion or discrimination. Harm reduction strategies are utilized by many people, including those with substance use disorders, members of their support network and even healthcare providers.
In the context of substance use, some commonly used harm reduction strategies include the provision of sterile needles or “Needle Exchange Programs,” needle collection boxes and naloxone distribution programs. Harm reduction strategies support the safety of all individuals by encouraging incremental changes to risky behavior.
The Syringe Exchange Program
Skagit County Public Health’s Mobile Syringe Exchange program aims to reduce health risks among adult IV drug users and the community at large. The program offers one-for-one needle exchange, safe disposal containers, no-cost Narcan® kits, education, referrals to treatment and more. Providing individuals with sterile needles helps prevent the transmission of blood-borne diseases, such as HIV and Hepatitis C. This program also helps reduce the number of contaminated needles in our community and the public waste system (i.e., in order to obtain a sterile needle, an individual must return a contaminated needle). An additional focus of the Mobile Syringe Exchange program is intervention and referral to behavioral health services, including treatment for substance use disorders. In 2021, 32 individuals were referred to treatment.

The Mobile Syringe Exchange program saves lives. It is estimated that 390 overdoses were reversed with naloxone obtained from the Syringe Exchange between February 2016 through December 2021.
The mobile van can be found in multiple locations throughout Skagit County:
| Mount Vernon | |
| Tuesday: 9AM-12PM | Coastal Farm & Ranch Parking Lot, 2021 Market Street |
| Thursday: 2PM-4PM | Senior Center, 1401 Cleveland Street |
| Sedro Woolley | |
| Tuesday: 1PM-4PM | United General Hospital, 2000 Hospital Drive |
| Thursday: 9AM-11AM | Senior Center, 715 Pacific Avenue |
| Burlington | |
| Thursday: 12PM-1:30PM | Tierra Nueva, 701 E. Fairhaven Avenue |
| Concrete | |
| 1st and 3rd Monday: 1PM-3PM | Senior Center, 45821 Railroad Avenue |
| Anacortes | |
| 3rd Monday: 10AM-11:30AM | Salvation Army, 3001 P Avenue |
| Marblemount | |
| 1st Monday: Call Randall for time and site | 360-826-2661 |
How to Prevention Infection, Overdose and Death
1. Prevent the risk of contracting communicable diseases by using clean needles. The Mobile Needle Exchange Program offers a 1:1 needle exchange along with other lifesaving resources.
2. Avoid an overdose by doing the following:
HOW TO AVOID AN OVERDOSE
DO NOT USE ALONE
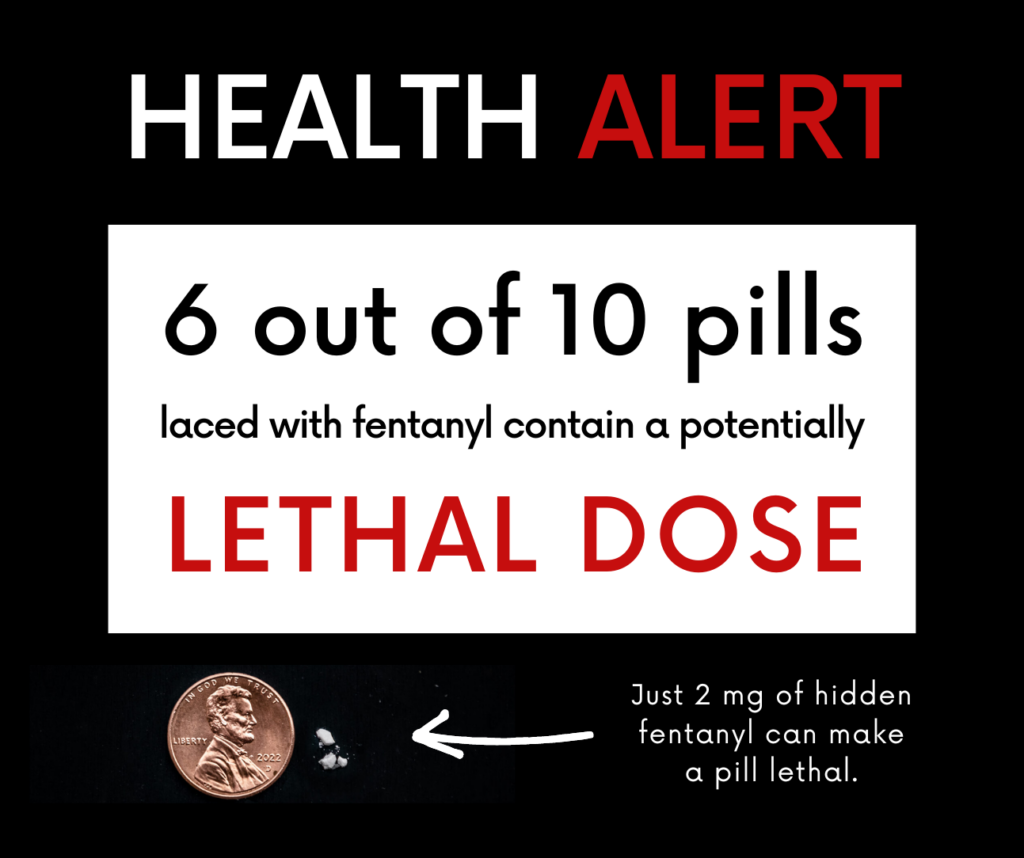
TEST FOR FENTANYL
Fentanyl test strips are available for free from Skagit County Public Health.
START WITH A SMALL AMOUNT
Fentanyl is approximately 50-100 times stronger than other opioids.
WATCH AND WAIT BEFORE THE NEXT PERSON USES
HAVE NALOXONE READY
Naloxone is available for free from Skagit County Public Health.
AN OVERDOSE IS A MEDICAL EMERGENCY-CALL 911 IMMEDIATELY
3. If you witness an overdose, call 911 immediately. YOU COULD SAVE A LIFE. The Good Samaritan Law protects you and the overdosing person from drug consumption or drug possession charges.
If you are unable to call 911 or unable to stay until medical help arrives, make sure to:
- Administer naloxone, if available.
- Provide rescue breathing.
- Leave the person where they can be found, with doors unlocked and/or open. If 911 is called, tell the dispatcher exactly where the overdosing person is. Give them as much information as possible (e.g. second floor or in the bathroom).
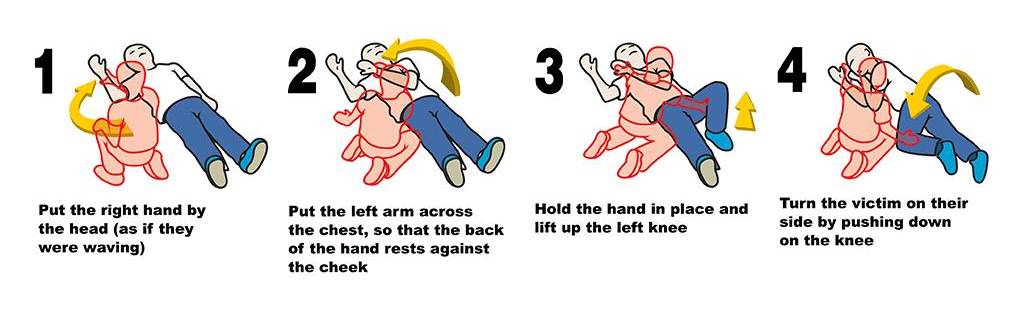
- Put the person experiencing an overdose in the Recovery Position. This will help keep their airway clear and prevent them from choking.
For more information and other harm reduction tips:
Overdose: Know the Signs and How to Help
Too much of an opioid—which varies based on the individual, length of time used and what the drug is made of, overwhelms brain receptors, and depresses the central nervous system. If an overdose is not reversed in time, a person’s body will shut down and breathing will stop. It can be difficult to tell if a person is just very high or experiencing an overdose. If you are having a hard time telling the difference, it is best to treat the situation like an overdose—it could save someone’s life.
Minutes count in an opioid overdose. Follow these steps:
1. Check for signs and symptoms of an opioid overdose.
 | Unconscious and/or Unresponsive |  | Blue/purple (light skin) or gray/ashy (dark skin) skin tone, nails, and lips |
 | Slow and shallow, erratic, or no breath |  | Cold and clammy |
 | Pinpoint pupils |  | Limp body |
 | Slow, erratic or absent pulse (heartbeat) |  | Vomiting |
 | Awake but unable to talk |  | Choking sounds or snore-like gurgling noises |
2. Call 911. Tell the dispatcher where you are and the symptoms of the person who has overdosed (e.g., not breathing or unconscious).
If you are trying to help in an overdose, WA State’s 911 Good Samaritan law protects you and the overdose victim from drug consumption or possession charges. Don’t be afraid to call 911 for help!
If you are unable to stay until medical help arrives, place the person on their side in a rescue position and where first responders can find them.
3. Give naloxone and rescue breathing.
If you have naloxone, give one dose. Naloxone can take 2-3 minutes to work, so start giving rescue breaths.
- Make sure nothing is in the person’s mouth blocking their airway.
- Place one hand on the chin and tilt the head back. With the other hand, pinch the nose closed.
- Administer a full breath and look for the chest to rise.
- Continue administering 1 breath every 5 seconds.
- If the person does not respond within 3-5 minutes, give a second dose of Naloxone and continue rescue breathing until medical help arrives.
4. If the person wakes up, stay with them. Encourage them to get follow-up medical care.
When naloxone wears off (roughly 30-90 minutes), a person may stop breathing again. Encourage the person to be taken to a clinic or emergency room where health care staff can monitor their breathing, manage any withdrawal symptoms, and treat any other medical conditions.
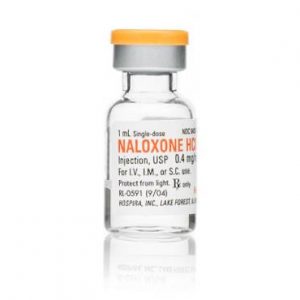
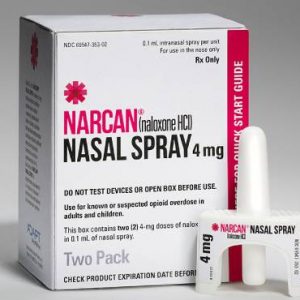
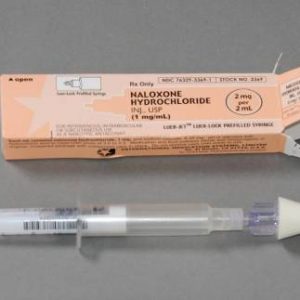
Carry Naloxone
Naloxone, also sold under the brand names Narcan® and Evizio®, is a lifesaving medication that can reverse an opioid overdose. Naloxone is not addictive, nor can it cause harm if administered in a situation that turns out to not be an opioid overdose. Anyone who either uses prescription or illicit opioids, or knows someone who does, should carry naloxone.
It is important to note that naloxone:
- Only works on opioids; it has no effect on someone who has not taken opioids
- Cannot be used to get high and is not addictive
- Has a long safety history; adverse side effects are rare
- Can be easily and safely administered by laypersons
Naloxone can be administered nasally or intramuscularly. There are currently four types of naloxone available; click each one to learn more.
Where to Find Naloxone
In Washington State, naloxone can be dispensed at pharmacies with or without a prescription. Naloxone can also be provided by community-based organizations.
No-cost naloxone can be obtained from the Mobile Syringe Exchange, didgwálič Wellness Center, and Skagit County Public Health.
Naloxone Providers:
| Provider | Address | Phone |
|---|---|---|
| Family Pharmacy (Skidmore Pharmacy) | 1213 24th St., S-400, Anacortes | 360-293-2124 / 360-293-0419 |
| Rite Aid #5234 | 1517 Commercial Ave., Anacortes | 360-293-2119 / 360-299-8568 |
| Safeway Pharmacy #0593 | 911 11th St., Anacortes | 360-293-5393 / 360-299-9135 |
| Walgreens #07131 | 909 17th St., Anacortes | 360-299-2816 / 360-299-8565 |
| Costco Pharmacy #662 | 1725 S Burlington Blvd., Burlington | 360-747-5702 / 360-757-5709 |
| Haggen Pharmacy #3436 | 757 Haggen Rd., Burlington | 360-814-1516 / 360-814-1595 |
| Walgreens #11300 | 623 S. Burlington Blvd., Burlington | 360-707-2741 / 360-707-5928 |
| Sea Mar Community Health Center Pharmacy | 7438 S. D Ave., Ste. C, Concrete | 360-853-8109 / 360-853-8350 |
| La Conner Drug #1146 | 708 E Morris St., La Conner | 360-466-3124 / 360-466-4775 |
| Hilltop Pharmacy LLC | 1223 E Division St., Mount Vernon | 360-428-1710 / 360-428-7847 |
| Sea Mar Community Health Center Pharmacy | 1400 N Laventure Rd., Mount Vernon | 360-428-4075 / 360-542-8797 |
| Haggen Pharmacy #3450 | 2601 E. Division St., Mount Vernon | 360-848-6930 / 360-848-6948 |
| Rite Aid #5245 | 412 E. College Way, Mount Vernon | 360-424-7958 / 360-424-0255 |
| Safeway Pharmacy #1472 | 315 E. College Way, Mount Vernon | 360-424-0467 / 360-424-0427 |
| Wal Mart Pharmacy 10-2596 | 2301 Freeway Dr., Mount Vernon | 360-428-3911 / 360-428-3688 |
| Rite Aid #5248 | 851 Moore St., Sedro-Woolley | 360-856-2153 / 360-856-0714 |
| Schaffner Pharmacy | 1990 Hospital Dr., Ste. 120, Sedro-Woolley | 360-853-2003 / 360-854-2765 |
| Walgreens #10994 | 320 Harrison St., Sedro-Woolley | 360-855-0735 / 360-855-0912 |
The Good Samaritan Law

If you witness what you think is an overdose, do not wait to call 911. The Good Samaritan Law protects you.
In WA State, anyone trying to help in a medical emergency is generally protected from civil liability by RCW 4.24.300. WA State’s 911 Good Samaritan Overdose Law (RCW 69.50.315) gives additional, specific protections against drug possession charges:
- If you seek medical assistance in a drug-related overdose, you cannot be prosecuted for drug possession.
- The overdose victim is also protected from drug possession charges.
- Anyone in WA State who might have or witness an opioid overdose is allowed to carry and administer naloxone. (RCW 69.41.095)
*The Good Samaritan Law does not protect those from outstanding warrants, probation or parole violations, drug manufacturing or delivery, controlled substances homicide, or crimes other than drug possession.
For further information and frequently asked questions, check out: